The uterus is the organ in which the fetus grows and is held during pregnancy. At the lower part of the uterus, just above the vagina, there is a narrow passage measuring 2-3 cm which consists of the cervix. Tumors that develop in this area usually start from the so-called transformation zone. This is the area where the endocervix, which is closest to the body of the uterus, meets with the ectocervix, namely, where the vagina meets with the cervix. Cervical cancer usually slowly develops over many years. Prior to the development of the cancer, it is common for tissues in the area to undergo cellular changes (known as dysplasia or precancerous lesions). It is important to know that at this initial precancerous stage, these dysplastic cells can be eliminated with simple interventions that can easily and quickly be performed at outpatient level.
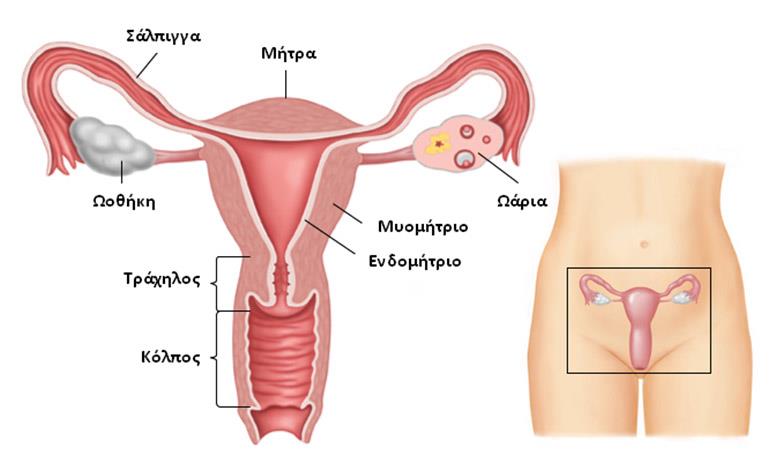
In the past, cervical cancer was one of the most serious gynecological cancers. Nowadays, thanks to early diagnosis with the well-known Pap test, the majority of women that are diagnosed in time will be treated.
EPIDEMIOLOGICAL DATA

Cervical cancer is the second most common cancer in the world. About 80% of cervical cancer cases occur in developing countries. In countries such as the USA, it is the eighth most common cancer. This difference is due to early diagnosis of the disease with the Pap test and early treatment. It is a remarkable fact that deaths from cervical cancer have been reduced by 75% in the last 50 years. In the European Union, the 2004 data showed 34000 new cases, while 16000 women died from the disease. Every woman is at risk of developing cervical cancer, whether they live in an urban or rural environment. However, women who belong to lower socioeconomic classes are at a higher risk.
ETIOLOGICAL FACTORS

The most significant risk factor for developing cervical cancer is the Human Papilloma Virus (HPV), which can be transmitted with sexual contact. The highly responsible HPV subtypes are 16 and 18. For the last 2 decades, it is known that HPV causes cervical dysplasia and other precancerous abnormalities, which can develop into cancer if not treated early.
Other risk factors include early experience of sexual intercourse, frequent change and large number of sexual partners, as well as poor physical and personal health which is associated with low socioeconomic living conditions. Also note that patients with a weakened immune system (e.g. AIDS or immunosuppressed patients) run the risk of developing cervical cancer.
PREVENTION
Documented knowledge that HPV constitutes the most significant risk factor is the development of cervical cancer led to the scientific discovery of a vaccine that protects against the HPV subtypes 6, 11, 16 and 18, which are responsible for 80% of the cervical cancers. The vaccine is recommended for girls and young women aged between 9-26 years, prior to their first sexual contact. To better understand the significance of the vaccination and its relationship with HPV, in the USA 25% of females aged 14-19 had been infected by the virus, while the rate soared to 45% for females aged 20-24. It should be noted that the vaccine does not protect against all the HPV subtypes and does not entail a change in the existing guidelines for a gynecological exam and Pap test every year, since this is the manner by which lesions are diagnosed and treated early. It should also be reminded that the use of a condom is mandatory not only for protection against HPV, but other sexually transmitted diseases as well.
SYMPTOMS

Cervical cancer is usual asymptomatic, especially in the early stages. Thus, it is imperative that you visit your gynecologist regularly (at least once a year) for a Pap test. When the disease is more advanced, the following symptoms may exist and an immediate medical assessment is needed.
- Pain or bleeding during or after sexual contact
- Unusual vaginal bleeding
- Unusual vaginal discharge
CAUTION: These symptoms could be due to various reasons and do not necessarily suggest the presence of malignancy. The basic rule is that they must be immediately examined by your gynecologist.
DIAGNOSIS

The Pap test is the easiest method used to detect dysplastic lesions and precancerous changes that could lead to cervical cancer if not treated.
- Biopsy: If changes are observed in the Pap test, your gynecologist will take a biopsy of a small tissue sample directly from the suspicious area and have it further examined.
- Cervical conization: In some cases a cone-shaped sample of tissue may be excised, which in the case of precancerous lesions is the final treatment.
- Cystoscopy, MRI of the lower abdomen, CT of the upper and lower abdomen: When there is a suspicion or we want to rule out advanced disease of neighboring or other organs, further tests may be requested.
TREATMENT

Treatment options primarily depend on the stage of the disease (tumor size, infiltration depth, spread of the disease to neighboring or other organs). Treatment methods include surgery, radiation therapy and chemotherapy.
Precancerous lesions and cervical cancer in situ: These lesions are premature and have not become infiltrative cancer. They can be completely treated using various techniques and by leaving the uterus intact.
These techniques include:
- Laser vaporization: This method uses a beam of light to destroy cancer cells.
- Loop excision: This method uses a wire loop heated by electric current to remove cells.
- Cervical conization: In this case a cone-shaped sample of tissue is excised, which includes the lesion.
Early-stage cervical cancer (Stages I-IIA): In cases where the lesion does not extend beyond the uterus, its removal (hysterectomy) with its surrounding tissue is usually the only treatment in some cases. The pelvic lymph nodes are also removed and examined for potential cancer cells. In the case of risk factors (lymph node infiltration, lymphatic vessel infiltration, or infiltration of tissues surrounding the uterus), then radiation therapy and chemotherapy must follow the hysterectomy.
Locally advanced cervical cancer (Stages ΙΙΒ-IVA): Where the disease spreads beyond the uterus to the neighboring tissues, surgery is not indicated. Based on the results of major clinical studies, radiation therapy is the primary therapeutic approach in locally advanced cervical cancer and is delivered in the form of combined external beam radiation therapy and brachytherapy (see below). In addition, in order to further enhance the radiotherapy results, platinum-based radiosensitized chemotherapy is administered weekly.
Stage IVB cervical cancer and recurrence: In cases where the disease spreads to remote organs (e.g. lungs, liver), the treatment options aim to relieve patients from the symptoms of disease by improving their quality of life and where possible extending the patients’ survival. Chemotherapy is the first therapeutic option. When the disease recurs in the pelvis, treatment is individualized and may include surgery, radiation therapy or brachytherapy, depending on whether the goal is complete treatment or symptom relief (pain, imminent-risk fistulas, etc.).
RADIATION THERAPY
Understanding Radiation Therapy
Radiation Oncologists use radiation to treat cancer, to control the size of the tumor, but also to relieve some symptoms, such as pain. Radiation acts on the cancer cell interior by destroying their ability to proliferate. When these cells die they are naturally discarded by the body. Healthy cells are also affected by the radiation, but unlike cancer cells, they are able to repair themselves from the damage that they have undergone.
External Beam Radiation Therapy (EBRT)
External beam radiation therapy is performed over a number of daily visits to our Center on an outpatient basis (without hospitalization).
EBRT uses high-energy X-rays (photons). The rays are produced by a linear accelerator, positioned at a distance from the patient’s body. Three Dimensional Conformal Radiotherapy (3D-CRT) is the most frequently used external beam radiation therapy technique, while Intensity Modulated Radiotherapy (IMRT), an improved version of 3D-CRT which focuses the dose on the target and avoids healthy tissues, has been increasingly gaining ground over recent years. The application of IMRT made using state-of-the-art and more precise image guided radiotherapy (IGRT) of the targeted area prior to the radiation therapy all the more necessary. Contemporary radiation therapy techniques have managed to reduce side effects to a minimum. Focusing on high-dose radiation on a tumor, with less impact on healthy organs thanks to IMRT, but also the safety that these doses will be precisely delivered to the target, thanks to IGRT, have established radiation therapy an extremely safe treatment method.
SIDE EFFECTS
Cervical cancer patients who are treated with radiation usually undergo radiosensitized chemotherapy at the same time. Side effects that may appear in the abdominal area during treatment are due to radiation therapy, while others (systemic) are due to chemotherapy.
- The most common radiation therapy side effects include diarrhea episodes, abdominal cramps, frequent urination, burning (stinging) sensation while urinating, skin irritation, nausea and feeling of fatigue. These symptoms are temporary and gradually subside within weeks of completing treatment.
- Chemotherapy side effects depend on the type of drugs used and will be discussed with your medical oncologist.
- These treatments may affect your ability to have children and this must be discussed with your doctor.
- The side effects are not the same for all patients and many of these may be controlled with medication or a change in your diet.
- Keep in mind that patients undergoing radiation therapy do not emit radiation themselves, so people who come into contact with them, including pregnant women or small children, are absolutely safe.
Caring for yourself during treatment
When patients undergo cancer treatments they are tried both physically and mentally. Take care of yourself:
- Get plenty of rest
- Follow medical instructions
- Eat a balanced diet
- Take care of your skin in the irradiated area
- Ask for help and support from family and friends, but also from cancer patient support groups
OUR APPROACH
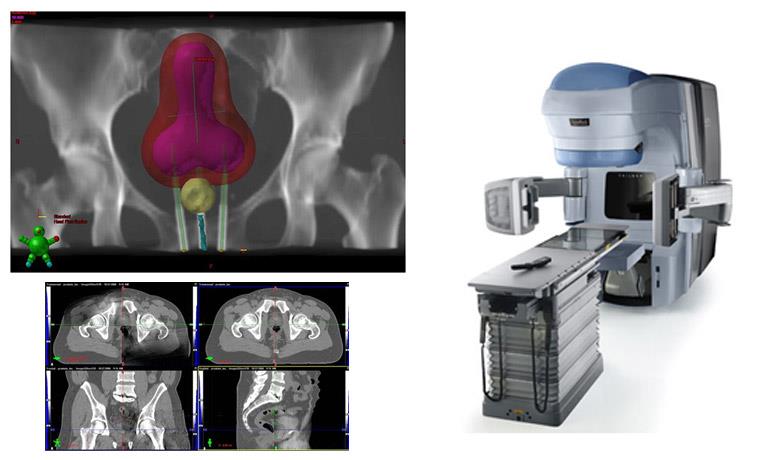
As soon as you visit the Metropolitan Hospital Radiation Oncology Center, you will be approached by a dedicated team of specialists, who will tailor the treatment to your individual needs. Other than radiation oncologists, this specialized team includes: the medical physics department, which consists of radiophysicists who specialize in the latest radiation therapy technologies, radiologic technologists, nursing and secretarial staff. Our team also works closely with all the medical specialties involved in cervical cancer, such as gynecologists, medical oncologists, but also radiologists and anatomic pathologists. This guarantees the most individualized, modern and effective treatment, with the least possible side-effects.
The state-of-the-art radiotherapy techniques and the skills acquired by the doctors from their training in centers of excellence in Europe and the USA ensure highly accurate and targeted tumor treatment, by delivering the maximum radiation dose possible, with the least damage to healthy cells.
At Metropolitan Hospital we offer state-of-the-art radiation therapy techniques to treat cervical cancer. These include:
- Three Dimensional Conformal Radiotherapy (3D-CRT)
- Intensity Modulated Radiotherapy - IMRT
- Image Guided Radiotherapy - IGRT
- Fusion of CT planning images with MRI images
- Fusion of CT planning images with MRI spectroscopy or PET-CT images
UNDERSTANDING BRACHYTHERAPY
The etymology of the word brachytherapy (brachy = short) refers to the position of the source of radiation, i.e. in or close to the tumor. This is a method by which radiation is performed from the inside and this distinguishes it from the widely-known external beam radiation therapy, where the source of radiation is outside the patient’s body.
Nowadays, brachytherapy is an effective therapeutic approach for many types of cancer. The therapeutic results of brachytherapy have either proven to be comparable with those of surgery and external beam radiation therapy, or improved when used in combination with these. The biggest advantage, however, is the minimization of side effects.
Over recent years, brachytherapy has become an integral part of gynecological cancer treatment, especially cervical cancer. A significant problem with conventional brachytherapy of the cervix is the insufficient delivery of an adequate dose to the parametria, thus, the larger the tumor in that area, the more the dose will be fractionated. With traditional radiation therapy methods, the clinical results for local control of stage IIB-IVA gynecological cancers was 30-80%, depending on the size of the tumors.
In recent years, the Medical University of Vienna and the Institute Gustave Roussy in Paris developed a method based on interstitial brachytherapy during which catheters are inserted in the parametria regions, where the tumor may have spread. The European Society for Radiotherapy and Oncology and the GYN GEC-ESTRO Working Group have published recommendations regarding the systematic performance of the method. With interstitial brachytherapy, slim catheters are implanted into the area of concern to mark the area to be irradiated. Targeted radiation is delivered with absolute accuracy and without exposing healthy tissue to more radiation that necessary, while the entire tumor is covered, irrespective of its shape and size.
In recent years, the integration of improved imaging methods (MRI) to brachytherapy planning has been boosted by the detailed three-dimensional (3D) multi-slice imaging of the topography of the pelvis and the tumor. This is a dynamic procedure used to monitor tumor response to the radiation over time (4D). This is translated as the best coverage of the tumor with maximum protection of healthy tissues.
Bibliography shows that with the systematic use of 4D MRI image-guided brachytherapy, the local control rates range between 85-100%, depending on the extent of the disease. Severe (Grade 3-4) delayed side effects of the gastrointestinal and urinary system do not exceed an overall rate of 5%.












































